Don’t hate me, but I take statins on the recommendation of my physician. This is not a suggestion that you should, but this is my story and my explanation for why I do.
I recently posted on my social media that I had increased my statin dose from 20 mg to 40 mg. I did this to support my longevity goals. I was surprised by the number of negative reactions I received. From the responses, one would have thought that I was going to drink gasoline!
Before I discuss why I decided (with my doctor’s support) to up my statin dose, I will discuss why this conversation is relevant. The number one cause of mortality worldwide and in the US is cardiovascular disease (CVD). (1) Cancer is a distant second. So, if we can understand the causes of CVD and use this understanding to help us mitigate the risks why shouldn’t we?
According to the Center for Disease Control, the most important risk factors for cardiovascular disease are: high blood pressure, elevated low-density lipoprotein cholesterol (LDL-C), diabetes, smoking and secondhand exposure to smoke, obesity, poor diet, and lack of physical activity. (2)
Although I’ve never smoked or had high blood pressure and have good body composition, exercise extensively and eat well, I have had high LDL-C levels throughout much of my adult life. Before treatment, my LDL-C levels averaged around 140 mg/dl and peaked at 180 mg/dl.
Twenty years ago, I resisted the advice of my doctors to take a statin to lower my LDL-C to under 100 mg/dl. Like many others, I did not want to take a drug that could have negative side effects. I believed that my elevated high density lipoprotein (HDL-C) was protecting me.
Ten years ago, I reluctantly began taking 5 mg of simvastatin daily. Eventually, based on the pleading of my doctor, we increased the dose to 10 mg. At 10 mg, my LDL-C averaged 120 mg/dl. A few years ago, I increased the dose to 20 mg without any noticeable side effects. This lowered my LDL-C to 100 mg/dl.
Based on my current understanding of the research, the decision to delay treatment and start with a low dose were probably not the best choices.
There is compelling evidence, and much of the medical community agrees, that an elevated LDL-C is a primary contributor to cardiovascular disease. A 2017 meta-analysis published in the European Heart Journal came to the following conclusion:
Meta-analyses (of over 200 studies) involving more than 300,000 participants and 80,000 Coronary Heart Disease (CHD) cases provide compelling evidence that LDL-C is causally associated with the risk of CVD (cardiovascular disease) and that the causal effect of LDL-C on CVD is largely independent of the mechanism by which LDL-C is ‘lowered’.
The article goes on to explain that lifetime exposure to elevated LDL-C is a causal component of cardiovascular disease. (3) Therefore, the earlier the treatment is started, the better.
Furthermore, the hypothesis that high levels of HDL-C is protective against CVD has not proven to be true. Study after study has failed to validate that higher levels of HDL-C provide protection against CVD. (4) (5) (6)
There are various pharmaceutical options for lowering LDL-C, each having different mechanisms of action, possible side effects, and costs. The most commonly used drugs are statins, Zetia (Ezetimibe) and PCSK9 inhibitors. (7) Statins have been around for over 30 years and now generics are available and affordable. PCSK9 inhibitors are newer drugs and are more expensive but are available when other options don’t work.
Statins work by blocking an enzyme that synthesizes cholesterol in the liver. Normally the liver synthesizes and deposits cholesterol inside carrier proteins that transport the cholesterol particles from the liver to other parts of the body via the blood stream. It should be stated that cholesterol is a necessary component of the cell membrane (cell wall) of cells and also serves as a precursor of various important hormones.
The problem with LDL cholesterol particles is that the cholesterol in LDL particles can adhere to the outer membrane (wall) of blood vessels in the heart (and other places in the body) and form plaques which can lead to narrowing of the vessels and eventually partial or complete blockage of blood flow.
The use of statins has saved many lives. Jennifer Robinson, a physician, professor of epidemiology in the University of Iowa College of Public Health, and co-author of a study that studied lipid (fat) lowering and cardiovascular outcomes determined that, annually, thousands of people with high LDL-C who take statins are spared a premature death. (8)
The main concern I had, and that many other people have, is the potential side effects of statins. The most common side effect reported is muscle soreness. According to the Mayo Clinic, approximately 5% of patients on statins will experience this side effect. The Mayo Clinic also lists other possible side effects including risk of diabetes, liver damage and neurological problems.
One respondent to my post on social media commented that within days of starting a statin they experienced significant muscle soreness. In this case, the solution is easy enough. Stop taking the statin but don’t give up on treating elevated LDL-C. Zetia is also cheap and has shown to be effective in many people.
There are doctors who suggest statin side effects occur at higher rates and are harsher than being reported. Dr. Aseem Malhotra is one such doctor although I have not seen any evidence supporting his claims. (9) It is noteworthy that many people in double blind trials report having muscle soreness when they are taking a placebo and not the actual drug.
Another argument I have heard against LDL-C treatment is having a zero or low calcium score. A calcium score is a test that estimates the amount of calcification in the coronary blood vessels. It is used as a short-term, two- to five-year, predictor of cardiovascular events. It is important to understand that a calcium score of zero does not necessarily indicate healthy arteries. (10) There can still be significant damage and inflammation to the arteries even with a calcium (CAC) score of zero as shown in the following diagram.
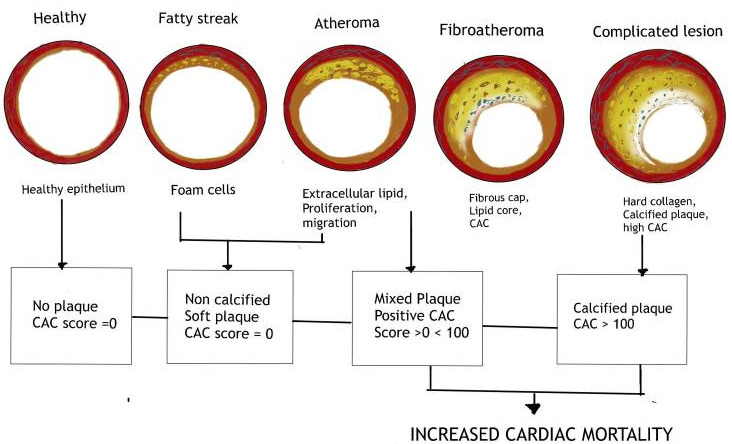
Given my history, my doctor and I decided to be more aggressive and get to the 70 mg/dl or lower level for LDL-C. Accordingly, I increased my dose to 20 mg of Atorvastatin twice a day. Doses of up to 80 mg per day are commonly used in practice.
Since my goal is to live a long and healthy life and not to necessarily to be drug-free, if medications, backed by science, can help me achieve my goal then by all means I will use them. Statin drugs can be an important tool for many people and therefore statins are not the boogie man and are not evil.
Remember that you alone are responsible for your health. If you want to live a long, healthy life and do not know your LDL-C level, I urge you to get tested soon. Getting the blood test is easy and cheap. In most states you can order it yourself without having to go through your doctor. With the right data and information, you can speak with your doctor more informed and be in the driver’s seat when it comes to your health and how to best achieve your health goals.
Written by Greg Damian: I am a 60-year-old author, motivational speaker, health and fitness disruptor and a coach. My book, Abs at 60: The Four Steps to Look and Feel Younger at Any Age was recently released on Amazon. My mission is to help 5000 people lose weight or to look and feel younger. I do this by applying my four step DOLR(TM) system that is described in the book. Each chapter has a set of questions for you to answer. You can download a free workbook that includes all of these questions at www.absat60.com
Written by Greg Damian. Edited by Mark Chavez MD, AKA The Health MD. Health Coaching and Concierge Physician practicing “Goal Directed Health and Longevity Medicine.” Inventor of The Gravity Ball Method of Grip-Free Resistance Exercise. Author of the book The 5 Habits of Healthy People.
References
- https://www.who.int/news-room/fact-sheets/detail/the-top-10-causes-of-death
- https://www.cdc.gov/chronicdisease/resources/publications/factsheets/heart-disease-stroke.htm
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5837225
- https://www.hsph.harvard.edu/news/features/why-good-cholesterol-may-not-always-be-good
- https://www.jacc.org/doi/10.1016/j.jacc.2022.09.027
- https://www.nih.gov/news-events/nih-research-matters/when-hdl-cholesterol-doesnt-protect-against-heart-disease
- https://www.mayoclinic.org/diseases-conditions/high-blood-cholesterol/in-depth/statin-side-effects/art-20046013
- https://now.uiowa.edu/2018/04/ui-study-statins-save-lives-people-high-levels-bad-cholesterol
- https://doctoraseem.com/the-great-statins-divide/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8723785



Kudos to you for working on your heart disease risk–most simply ignore it or complain about it. Statins have gotten a bad rap–I worked as a registered dietitian for over 25 years(now retired) so I have seen firsthand what heart disease does. One must also know the genetic risk factors–I have them, and take a low dose of 10 mg of a statin to get my numbers to the right place. The REST is lifestyle management.
Thanks for your comment Marilyn.